Cancer treatment is evolving at breakneck speed. What once relied heavily on surgery, chemotherapy, and radiation is now being joined — and sometimes replaced — by highly advanced, precision-driven therapies. These innovations leverage biology, engineering, data science, and immunology in unprecedented ways. Here, we explore the most promising recent and emerging technologies that are reshaping how we fight cancer.
1. Immunotherapy: The Immune System as a Weapon
Immunotherapy remains one of the most transformative areas in oncology. Rather than simply killing cancer cells directly, these therapies empower the patient’s own immune system to recognize and destroy tumors.
CAR-T & CAR-NK Cell Therapies
- CAR-T cells (Chimeric Antigen Receptor T-cells) are genetically engineered T-cells that specifically target cancer antigens. Recent trials are expanding into solid tumors, despite CAR-T’s success in blood cancers. A new clinical trial showed that CAR-T therapy improved survival in patients with advanced gastric or gastro-oesophageal junction cancers by about 40% compared to standard care.
- CAR-NK cells are another exciting offshoot. NK (Natural Killer) cells are engineered with CARs to target cancer. These may have advantages over CAR-T in terms of safety (reduced risk of certain side-effects) and potential for “off-the-shelf” therapies.
Tumor-Derived and Cell-Based Therapies
- Lifileucel: This is the first tumor-derived T-cell therapy approved for metastatic melanoma.
- Dendritic cell-based vaccines: Dendritic cells, which present antigens to other immune cells, are being used to create vaccines that train the immune system to attack cancer cells.
2. Personalized Cancer Vaccines (mRNA & Neoantigen-Based)
- Vaccine technology — made famous by COVID-19 — is now being applied to cancer in novel ways.
- BioNTech and Genentech created the personalized mRNA vaccine known as Autogene Cevumeran. It uses mRNA to encode neoantigens — tumor-specific mutated proteins — identified in a patient’s tumor, to elicit a tailored immune attack.
- mRNA-4157 / V940: Another mRNA-based cancer vaccine, encapsulated in lipid nanoparticles, which is being tested in combination with immune checkpoint inhibitors.
There is also a growing number of clinical trials around mRNA cancer therapies, including in China, which has approved a synthetic mRNA cancer treatment for trial use.
Reuters
These customized vaccines can boost the immune system in a very specific way and may be less toxic than conventional treatments.
3. Nanotechnology & Nanomedicine
In cancer treatment, nanotechnology has opened new doors for drug delivery, imaging, and immune modulation.
- A 2025 review highlights how nanoparticles are being designed to deliver immunotherapy agents directly to tumors, improving their effectiveness and limiting side effects.
- Theranostic nanoparticles combine therapy + diagnostics — they can carry a drug and, at the same time, provide imaging feedback. This helps in tracking how well the therapy is working in real time.
- Photoimmunotherapy, which uses light to activate immune-stimulating nanoparticles, and radioimmunotherapy also make use of advanced nanoplatforms, allowing for extremely precise and targeted cancer treatment.
4. Precision Medicine & AI-Driven Oncology
Data science is playing a major role in making cancer treatment more personalized than ever.
- AI & Machine Learning for Treatment Planning
- AI is being used for adaptive radiotherapy planning, where treatment plans are recalculated in real time based on daily imaging. Radiation will only be directed at the tumor as a result of this, sparing healthy tissue. In precision oncology, AI models analyze multi-omics data (genomics, transcriptomics, etc.) to recommend tailored therapies.
- In addition, research has been conducted on reinforcement-learning-based decision support systems that have the potential to dynamically optimize radiopharmaceutical therapy for specific patients. AI in Imaging & Diagnostics
- AI helps in reading histopathology slides (tissue images), detecting subtle features that might be missed by human eyes.
Combined with new imaging modalities, AI is also improving motion management in radiotherapy (detecting how tumors move during treatment), thereby increasing precision while reducing collateral damage.
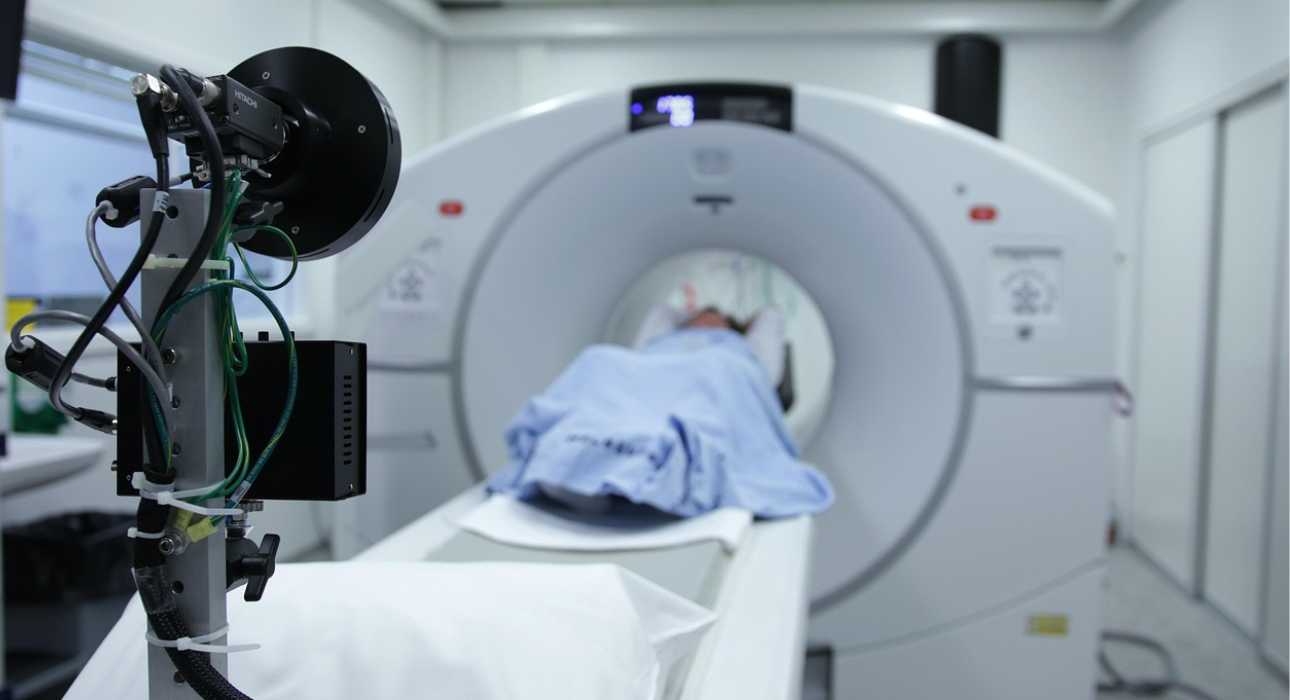
5. Advanced Radiotherapy: From Imaging to Treatment
Radiotherapy itself is being revolutionized by newer imaging technologies and smarter delivery systems.
- Photon-Counting CT (PCCT): This is a cutting-edge imaging technique with better spatial resolution, lower dose, and richer data. In radiotherapy, PCCT helps in more precise tumor delineation, better dose calculation, and more accurate monitoring of treatment response.
- Theranostics & Radiopharmaceuticals: These are radioactive drugs that both image (diagnose) and treat cancer. Combining them with AI and molecular data can personalize dosages and improve efficacy.
Integration & Future Outlook
The most exciting thing about these technologies is not just individual advances, but how they are combining:
- AI, nanotechnology, and immunotherapy: AI can design better nanoparticles and predict how a patient’s body will react to immune therapies.
- Multi-omics Decision Support: AI systems, trained on genomics, proteomics, and patient history, can help oncologists choose the best treatment path in real time.
- Personalized Vaccines + Cell Therapies: mRNA vaccines can prime the immune system, while CAR-T or CAR-NK cells can deliver a powerful, targeted attack.
According to experts, the future of cancer treatment will be highly personalized, minimally invasive, and data-driven
Challenges & Ethical Considerations
While these innovations are promising, they come with important challenges:
- Cost & Accessibility: Many of these therapies are extremely expensive to develop and administer, which raises concerns about equitable access.
- Safety Risks: New therapies (like engineered cells or gene editing) could have side effects — such as immune overreaction or genetic off-target effects.
- Regulatory Hurdles: Approval processes for personalized and genetically engineered therapies are complex and slow.
- Data Privacy: AI-driven oncology relies heavily on patient data (genomes, imaging, clinical records), raising serious privacy concerns.
- Manufacturing: Scaling cell therapies (like CAR-T or dendritic vaccines) for wide patient populations remains a logistical and technical challenge.
Conclusion: A New Dawn in Cancer Treatment
The way cancer is treated is changing fundamentally. The future is clearly leaning toward tailored, intelligent, and synergistic treatments rather than generic ones. The convergence of immunotherapy, nanotechnology, AI, and gene editing is not just theoretical — many of these approaches are already in clinical trials or early use.
Cancer may remain one of the toughest medical challenges, but the technological arsenal available today gives genuine hope. As researchers, clinicians, and companies push forward, the dream of more effective, less toxic, and highly personalized cancer therapy is becoming an increasingly real possibility.